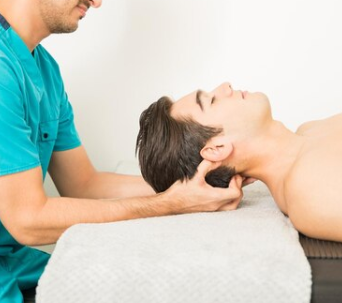
Is joint pain connected to the weather? Many people are surprised when their knees ache before it rains, or when their back feels tight on cold mornings. At PhysioNow, we hear these concerns every single week, especially during seasonal transitions in Canada. Us Canadians know just how our weather can swing back and forth. While some people assume it’s “just age” or “just arthritis,” the truth is more complex: Weather changes can genuinely influence your joints, muscles, and nervous system. Importantly, this does not mean your joints are damaged. Rather, it means your body is reacting to subtle environmental changes, something completely normal and highly treatable with physiotherapy.
How does weather affect muscle and joint pain?
Your body is constantly adapting to changes around it. Namely, temperature, pressure, humidity, and even sunlight. Naturally, when these factors shift suddenly, your tissues response does too. This can lead to temporary stiffness, increased sensitivity, or a flare-up of older injuries. Arthritis.org has a great article on the best climates for arthritic joints.
1. Barometric pressure
Before rain or storms this pressure drops, causing the tissues around your joints to expand slightly. Even tiny changes in pressure can irritate inflamed or old injuries. This may result in:
- Achy, throbbing pain
- Increased stiffness
- Sensitivity in arthritic joints
- Old injuries feeling “reactivated”
2. Colder temperatures
Aditionally, cold temperatures also plays a role by decreasing blood flow, so muscles naturally contract to preserve heat. Tendons and ligaments become less flexible, making movements feel stiff or uncomfortable. As an example, you may feel:
- Tight lower back
- Stiff neck and shoulders
- Knee and hip pain
- Increased stiffness and less flexibility in joints and muscles
- Susceptibility to injuries when exercising “cold”
3. Humidity/dampness
Humidity and damp weather can further aggravate the soft tissues, especially in individuals with chronic inflammation or scar tissue from past injuries. These tissues absorb moisture from the air, which can make them swell or feel heavy. This may lead to:
- Heaviness or swelling in the joints
- Increased dull aching
- Reduced mobility
- Pain in hands, knees, and spine
4. Rapid changes in temperature
Lastly, rapid weather changes can influence your nervous system. A sensitive nervous system may interpret small environmental changes as pain or discomfort, especially if you already live with chronic pain, fatigue, or stress. Some of the symptoms may include:
- Pain flare-ups
- Muscle tension
- Fatigue
- Restless sleep
- Feeling more “inflamed” or sore than usual
Who is more likely to get joint pain from weather changes?

Not everyone reacts the same way to weather. Fortunately, some patients barely notice changes, while others feel it intensely. A lot of factors go into it, such as your joint condition, lifestyle, muscle strength, inflammation levels, and nervous system sensitivity. You’re more likely to feel weather-related pain if you have:
- Osteoarthritis (knees, hips, hands, spine)
- Previous fracture
- Chronic pain (greater than 3 months)
- Sedentary lifestyle (more stiffness)
- Comorbid conditions such as fibromyalgia
- Older sports injuries (strains, sprains etc)
- Sleep issues or high stress
Your body is simply giving you signals, not warning signs of damage, but reminders that your joints need more support, movement, and strength. This is where some guided rehabilitation with a professional can help you recover.
What can physiotherapy do for my joint pain?
Physiotherapy is one of the most effective ways to manage and prevent weather-related joint pain. At PhysioNow, our therapists take a full-body approach: improving joint mobility, strengthening muscles, calming the nervous system, and teaching you how to manage flare-ups independently. Here are the main ways physiotherapy helps:
1. Joint mobilizations and soft tissue work
Gentle hands-on techniques restore smooth joint movements and can address muscle tension. This can lead to:
- Less pressure inside joints
- Improved lubrication
- Reduced pain and tightness
- Better range of motion
2. Strengthening
Strong muscles lead to healthy joints. Regular strength training has a whole host of benefits not only for reducing current pain but preventing future issues as well.
3. Nervous system calming techniques
As we discussed, weather affects the nervous system as much as the joints. Physiotherapists may include
- Diaphragmatic breathing
- Breath work coordinated with exercises
- Mindfulness techniques
- Education on pain control strategies
- Massage techniques
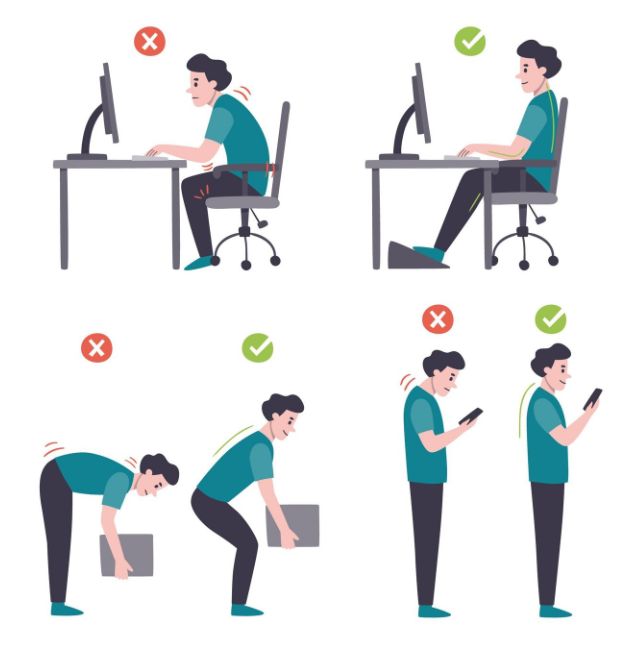
4. Posture and movement correction
Poor posture or movement patterns puts extra stress on joints, making them more susceptible to weather-based changes. Your physiotherapist will observe and correct:
- Sitting/desk work posture
- Walking mechanics
- Standing alignment
- Sleeping positions
- Lifting technique
- Sports specific movements
5. Personalized flare-up management plan
Every patient receives an individualized plan for weather-sensitive days. It will address your specific concerns, circumstances, and goals. This may include your exercise routine, lifestyle advice, and other joint protection strategies.
When should I seek help?
You should book an assessment if:
- Weather changes trigger your pain
- Your joints feel stiff most mornings
- You avoid activity on cold days
- Pain affects sleep or your mood
- You rely on painkillers frequently
- Old injuries flare up every season
Pain is not something you have to “just live with.” Fortunately, there is help. Look for PhysioNow in one of our 10 locations across the west GTA to get started with your recovery! We provide quality Physiotherapy services for Burlington, Oakville, Mississauga and Etobicoke. Whether it is a fracture, neck pain, back pain, and old sports injury, or you have no idea where the issue came from, we can help! Book with PhysioNow today for your first assessment and treatment!