Pelvic health physiotherapy is a specialization that focuses exclusively on the pelvic floor. This includes conditions such as incontinence, pelvic pain, sexual dysfunction, pelvic organ prolapse and more!
Treatment of the pelvic floor muscles and structures is both like, and unlike the other areas of the body. For example, just like any other muscle, they can be strong or weak, lengthened or tight, hypermobile or hypomobile. On the other hand, treatment of the pelvic area may require some unique techniques and unique tools during treatment. One of these tools is called a pessary.
What are pessaries used for?
A pessary is a medical device typically used to help manage pelvic floor dysfunction, particularly in conditions like pelvic organ prolapse, urinary incontinence, and stress incontinence. It’s a device that is inserted into the vagina to support the pelvic organs and help alleviate symptoms. Oftentimes, it is the missing piece for many individuals managing pelvic floor prolapse, stress incontinence and even plays a role in prevention of recurrent UTI`s (urinary tract infections).
How do I know if I need a pessary for my condition?
A pelvic floor physiotherapist specializes in assessing, diagnosing, and treating pelvic floor dysfunctions. They use various techniques, including exercises, manual therapy, and education, to help individuals strengthen or relax the pelvic floor muscles. Their expertise can support individuals in improving bladder and bowel control, sexual health, and overall pelvic function.
During a session, they will do a comprehensive examination to identify the root cause of your condition. They will use this information to create a unique treatment plan for you to address your needs and goals. Your Physiotherapist will discuss this plan with you including if they think you would benefit from a pessary, and what kind of pessary.
Types of pessaries
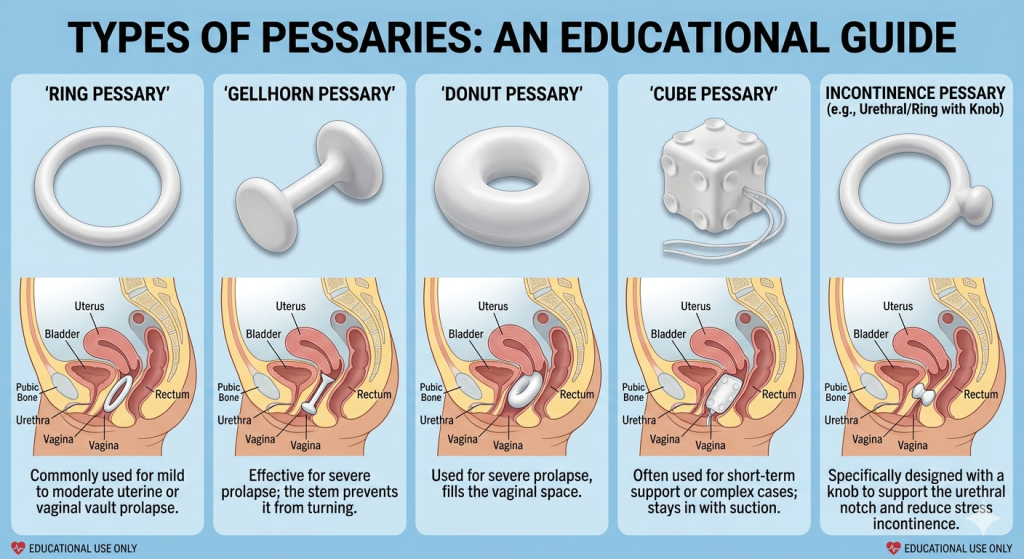
There are different types of pessaries that can be used for different pelvic floor conditions. Decisions on which type is needed are determined by the type and severity of the condition, as well as how well you can manage them on your own. These include but are not limited to:
Ring pessary: It is commonly used for stress incontinence and mild pelvic organ prolapse. Benefits include being very easy to put on and take off by yourself
Gellhorn pessary: It is used for moderate to severe pelvic organ prolapse
Cube pessary: Used for third dergree pelvic organ prolapse
Donut pessary: Used for prolapses needing more support
Inflatable pessary: These are more like custom fit and are used for advanced prolapse conditions
Gehrung pessary: For rectocele (rectum prolapse) and cystocele (bladder prolapse)
Why do I need a pessary if I am already doing pelvic floor physiotherapy?
Pessaries are a teammate in your pelvic floor rehabilitation. Namely, pessaries stops the leak and heavyness instantly. This gives you the confidence to return to activities such as running, lifting and long term muscle strength training.
A pessary gives support to the prolapsing organ and let your muscle train effectively during exercises. Also, it helps to prevent the prolapse from getting worse due to repeated intra-abdominal pressure (such as when you brace during exercises). From the top down, pessaries help your brain find your pelvic floor muscles making your rehabilitation exercises more targeted and successful.
Additionally, your physiotherapist will do the following:
1. Assessment and fitting of pessaries: A pelvic floor physiotherapist may assist in the fitting of a pessary. They can determine if it’s the right solution for you and help with proper size, shape, type and insertion and comfort.
2. Pelvic floor rehabilitation: After fitting a pessary, a pelvic floor physiotherapist can guide you through exercises and techniques to strengthen or relax the pelvic floor muscles. This can enhance the benefits of the pessary and help with the underlying causes of pelvic floor dysfunction.
3. Education: Your physiotherapist will educate you on pelvic floor health, how to care for the pessary, and when to seek further help. Your therapist will teach you how to insert, remove, and clean it so that you can have a total control of your care.
Pessary myths
1. Have to wear it all day
You don’t have to wear a pessary all day, wear it only for high impact actvities or if you are on your feet for long durations
2. It is only for old women
People of all ages wear pessaries including postpartum womenand those who wish to delay surgeries
3. I can`t have sex with it
While some types of pessaries must be removed, many common types such as ring pessaries are safe to keep in
Looking for pelvic pain, prolapse, or pessary help?
Then look for PhysioNow! A pessary does not fix the prolapse but it manages the symptoms in a way that you can eliminate the need to do the surgery. With an active physiotherapy program paired with the pessary, you can actively rehabilitate your body with the best possible support. Physionow has expert pelvic health physiotherapists ready to help you. We have 10 locations across the west GTA from Burlington, Oakville, Mississauga to Etobicoke, to assist you. Start your road to recovery, book with PhysioNow today for your first assessment and treatment!