Soccer is a demanding sport. The quick sprints, sudden pivots, and powerful kicks that make the game exciting also put a lot of stress on your body. As the weather starts to warm up in the GTA, we know more of you will be getting outside and returning to the field. As a result, we always expect to see more injuries during this time, especially for our soccer players. Here’s what you need to know about soccer injury rehab, and how to stay off the sidelines this spring and summer.
Why do injuries happen at the start of the season?

Understanding why injuries happen is important to preventing them. Injuries usually stem from mechanical overload (too much force at one moment), training overload, (too much activity over time), pre-existing imbalances and injuries, and improper gear or technique. Let’s discuss each one briefly.
- Mechanical overload
- Soccer has a lot of high speed movements like kicking and sprinting. In these movements, huge amounts of force are generated in the tissues in a very short amount of time. Because of this, this is often where they are the most vulnerable to strains and sprains.
- Training overload
- In other words, doing too much, too soon. If you go from the couch to a 90-minute match without a progressive build-up, your tissues might not be ready for the load
- Muscular imbalances and old injuries
- It could be as simple as an old twisted ankle that you never rehabbed. As a result, it’s not as stable or strong as it should be, leaving it and other areas vulnerable to injury
- Gear and technique
- Having ill fitting or worn out shoes can increase the risk of falls, slips, and other traumas. Having improper technique such as with kicking the ball can put excessive strain on muscles and joints.
What are the most common soccer injuries?
Because soccer involves constant change of direction and explosive movements, most injuries affect the lower body. Here are the most common ones that we see in the clinic:
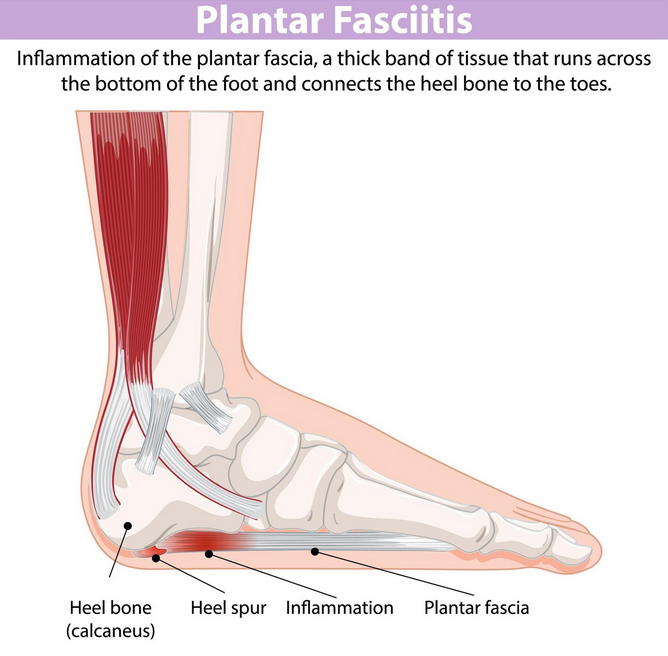
- Ankle sprains: Usually caused by rolling the ankle on uneven turf
- Hamstring strains: Often happen during a full-out sprint or a high kick
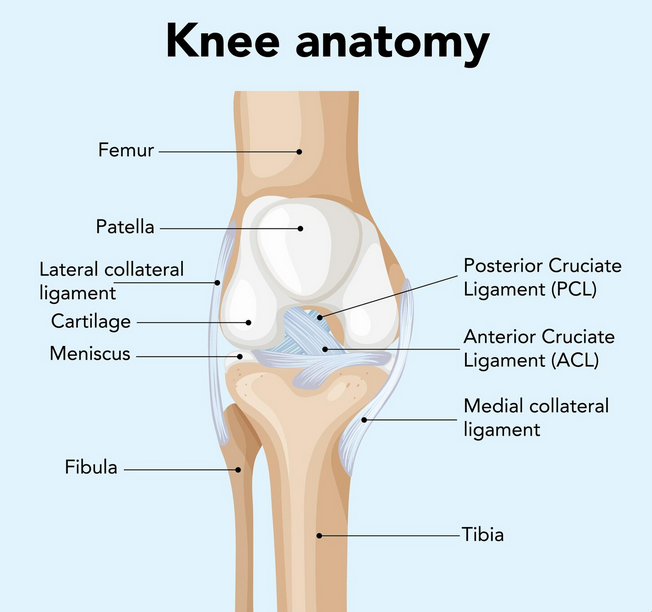
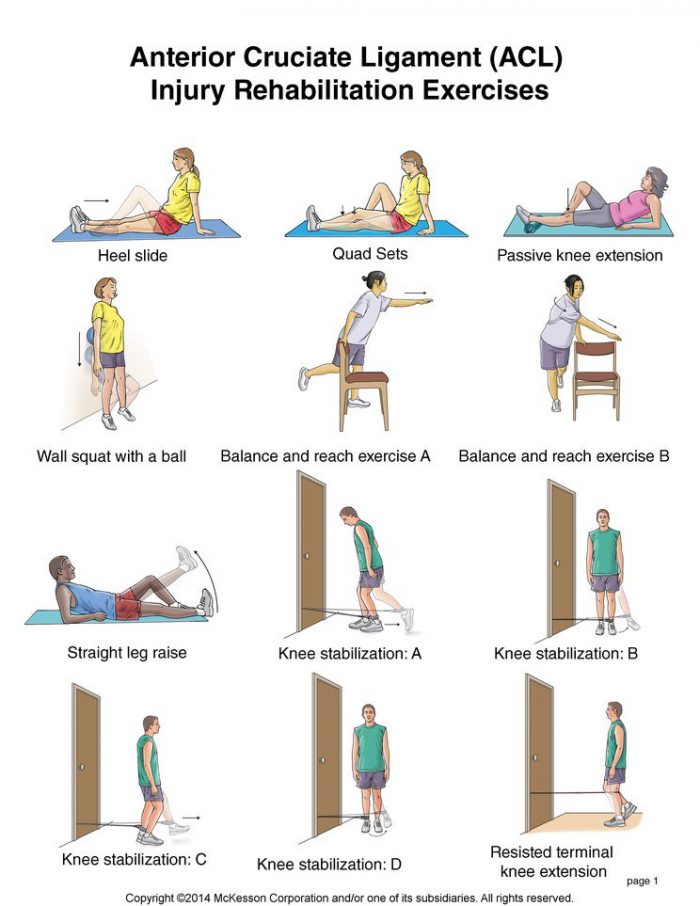
- ACL Tears/Knee sprains: These frequently occur from a sudden pivot or change in direction.
- Groin pulls: Common when changing direction quickly or reaching for a ball.
- Shin splints: An overuse injury often felt by players increasing their duration of play or playing on hard surfaces.
Soccer injury rehab and prehab
Physiotherapy doesn’t just tell you to rest and ice. It can help even before you’re injured in a new mindset known as prehab.
What is prehab?
The best injury to treat is the one that never happens. Prehab, short for prehabilitation involves:
- Screening: Identifying your specific movement impairments to address areas of risk
- Strength & balance: Building “bulletproof” joints that can resist common injury patterns
- Sport specific drills: Improving your body’s ability to decelerate, pivot, and other soccer techniques
What is rehab?
If you’re already hurt, we focus on a phased return to play. We aim to get you back as quickly and as safely as possible. There is no reason to rush a return if it will only result in another, and potentially more severe injury.
- Phase 1: Pain management: Using manual therapy, heat, ice, and gentle movement to reduce swelling and regain range of motion
- Phase 2: Loading: Gradually introducing weight and resistance to the injured tissue so it learns to handle stressors again
- Phase 3: The final push: This is where we get sport-specific. We’ll have you sprinting, jumping, and kicking in a controlled environment to ensure you’re 100% ready for game day.
Need help with soccer rehab or a sports injury?
Then look for PhysioNow! We have an expert team of health professionals ready to help you get back into the game. Whether you’re preparing for the season or looking to rehab an injury prior to starting, we’ve got you.
We have locations at 10 clinics across the West GTA including Burlington, Oakville, Missisauga, and Etobicoke. With extended evening hours, Saturday hours, and free parking, we make sure that our clinics are accessible for everyone. Don’t let your pains stop your participation this summer, get it treated fast! Book with PhysioNow today for your first assessment and treatment! Or find us at P: 289-724-0448 or Email: applewood@physionow.ca