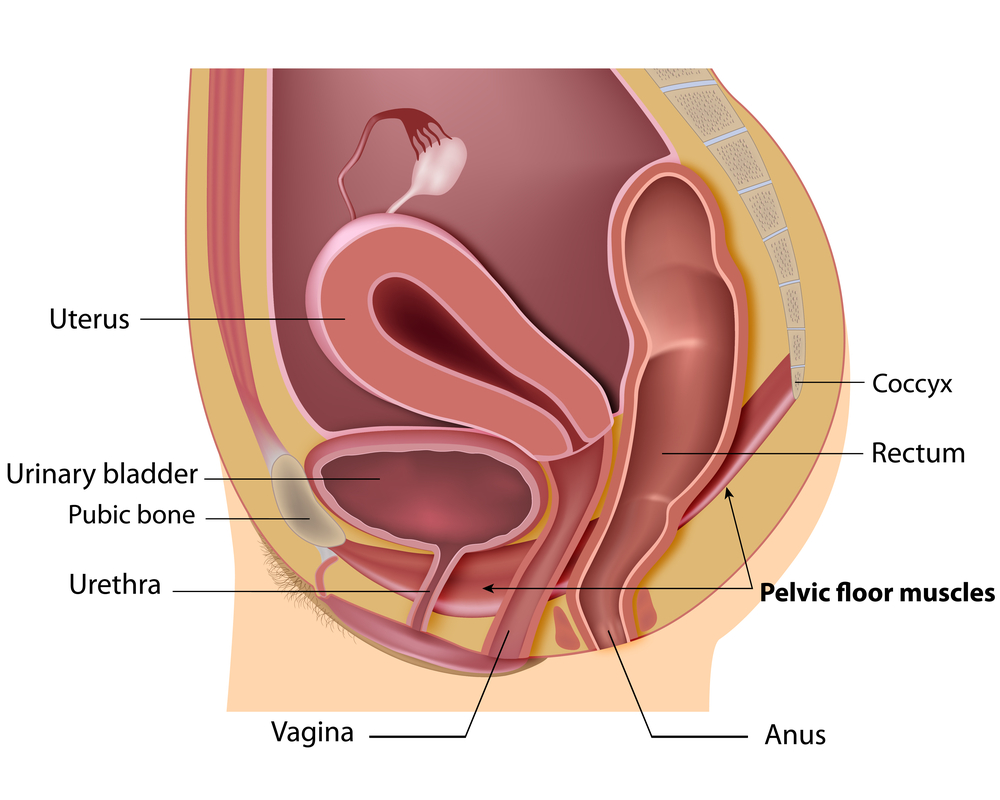
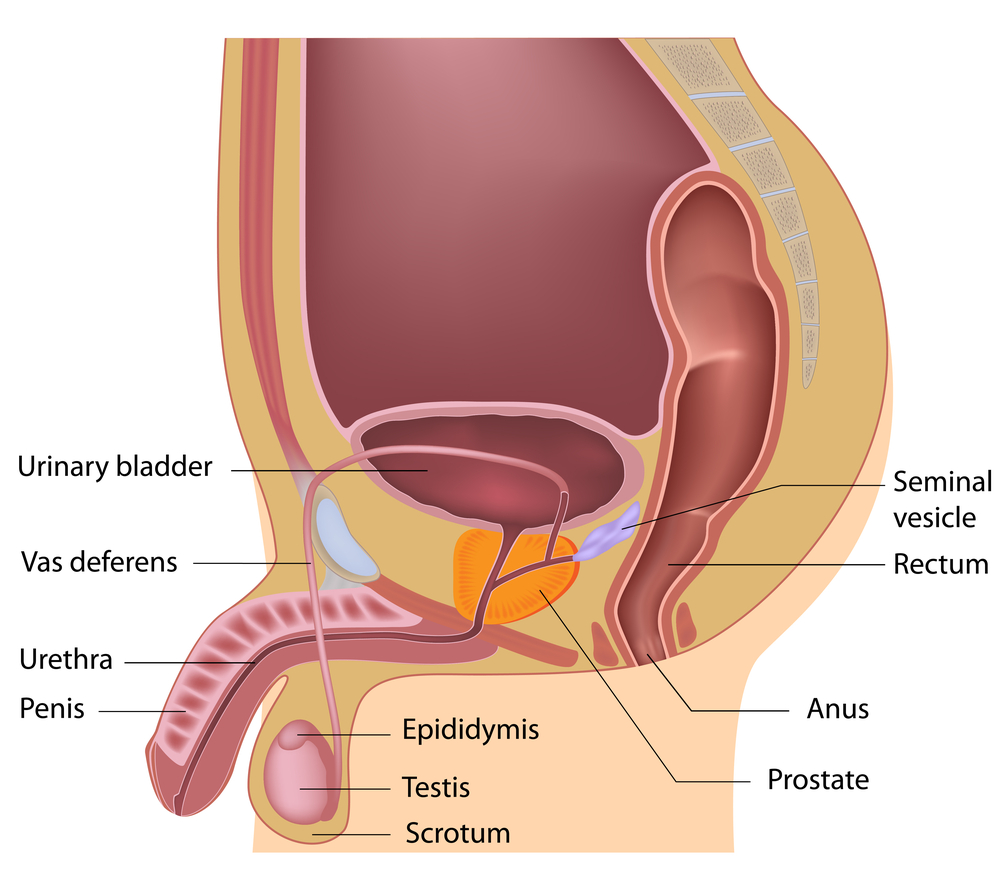
Dyspareunia and Physiotherapy

Dyspareunia is genital pain experienced by women just before, during or after sexual intercourse. Some women have always experienced pain with intercourse from their very first attempt. Other women begin to feel pain with intercourse or cyclically with menstruation. They can also have pain after an injury or infection . Sometimes the pain increases over time. When pain occurs, the woman may be distracted from feeling pleasure and excitement.
Causes
• vaginal dryness from menopause, childbirth, breastfeeding, medications
• skin disorders that cause ulcers, cracks, itching, or burning
• infections, such as yeast or urinary tract infections
• spontaneous tightening of the muscles of the vaginal wall
• endometriosis
• pelvic inflammatory disease
• uterine fibroids
• irritable bowel syndrome
• radiation and chemotherapy
Other factors that affect a woman’s ability to become aroused can also cause dyspareunia.
These factors include:
• stress, which can result in tightened muscles of the pelvic floor
• fear, guilt, or shame related to sex
• self-image or body issues
• medications such as birth control pills
• relationship problems
• cancer, arthritis, diabetes, and thyroid disease
• history of sexual abuse
Symptoms of Dyspareunia
• Pain while inserting a tampon or during penis penetration
• Pain with certain sexual partners
• Deep pain during thrusting
• Burning pain or aching pain
• Throbbing pain, lasting hours after intercourse
Check out this link for more information.
Physiotherapy Treatment for Dyspareunia
Education:
To help describe how the pelvic floor muscles can cause pain. Education can also provide techniques that can be used at home.
Manual Physiotherapy: to mobilise muscle and soft tissue, normalize overactive muscles, improve circulation and desensitize painful areas.
Desensitization therapy: learning vaginal relaxation techniques, such as Kegel exercises, that can decrease pain.
Sex therapy: learning how to re-establish intimacy and improve communication with your partner.
Water-based lubricants rather than petroleum jelly or other oil-based lubricants are preferable. Oil-based lubricants tend to dry the vagina.
Psychologic therapies: Cognitive-behavioral therapy and mindfulness-based cognitive therapy can be helpful.
Pelvic muscle relaxation exercises: used with biofeedback, this can help women with tight pelvic muscles learn to consciously relax tight muscles.
If you or someone you know suffers from dyspareunia, please call today to get started on Physiotherapy treatment! We can help at PhysioNow. Often only a few visits with our specially trained Phyiotherapist can help to get you on the road to recovery.