Motor Vehicle Accidents / MVA and physiotherapy.
Injuries sustained from a motor vehicle accident affect your normal function in life differently. It depends on the extent of the impact. Thus, it is very important to address any pertaining issues from the accident to your doctor. Additionally, to start rehabilitation at the earliest to decrease the impact of injury and its effects.
MVA injuries can be as minor as sprains or strains or it can be extensive that might include concussion, fractures, neurological involvement, other musculoskeletal involvements, etc.
Once you are involved in an accident and you are discharged from your preliminary care, you would contact your auto insurance company for guidance on starting physiotherapy sessions.
Physiotherapy sessions for a motor vehicle accident:
Once you decide to attend a physiotherapy clinic, these are the few things to do and to expect on your first visit.
- Book an appointment in a clinic which you decide to proceed with.
- Once you arrive expect to fill a few Auto insurance forms and clinic specific forms to start your assessment at the clinic.
- You would be seeing a physiotherapist who could be your primary care provider.
- The therapist would do a detailed assessment on your situation and would also go over your treatment plan pertaining to your injury.
- Your treatment session would be patient specific and progressive to get back to your normal functionality.
Facts about your treatment plan and coverage:
Once you are in a motor vehicle accident, you are mostly covered by the auto insurance company for treatment sessions.
Your treatment coverage depends on the category that you fall into.
- Minor injury guideline/ MIG, where your injury falls into the category of sprains and strains and would need a shorter duration of recovery and treatment sessions. Your treatment sessions could extent up to 4 months or as needed. Reassessments are done as needed to see your progress and to plan further with your sessions.
- Out of Minor injury guideline, where your injury is more extensive or catastrophic. Where the duration of recovery is longer and so the treatment allotment is longer when compared to MIG.
- Any multidisciplinary approach needed would be advised and would be recommended to your insurance company for further proceedings.
Commonly seen injuries after a motor vehicle accident:
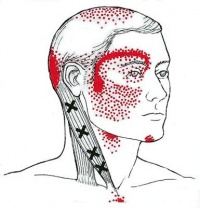
- Whiplash injury to the neck: which can include one or more of the symptoms ; pain, stiffness, swelling, muscle spasm, headaches, tingling /numbness into the hands, weakness, difficulty sleeping.
- Low back Sprain/ strain or disc related symptoms which includes, pain, stiffness, tingling and numbness into the leg, disturbed sleep.
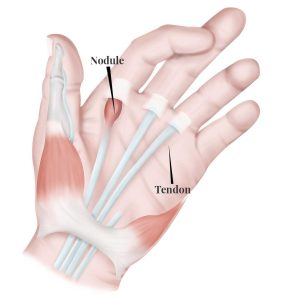
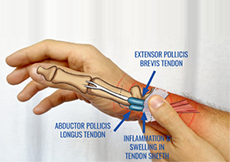
- Shoulder, elbow, wrist, hip, knee, ankle sprain/ strain.
- Seatbelt or airbag related pains in the chest area and abdominal area.
- Fractures.
- Concussion symptoms which might include dizziness, headaches, light and noise sensitivity, blurred vision, nausea, issues with concentration, imbalance, weakness, slurred speech, anxiety, depression, etc.
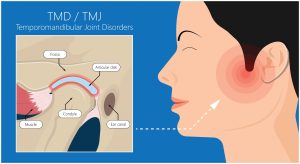
- Vestibular symptoms with symptoms such as dizziness, nausea, vomiting, difficulty with positional changes, sense of imbalance, etc.
Treatment sessions:
These are patient specific.
- Electrical modalities such as IFC, TENS, Ultrasound, LASER, heat or cold packs for pain relief and decreasing muscle spasm, and to improve circulation to the area.
- Manual therapy which includes soft tissue techniques, joint mobilization, joint traction. Muscle energy techniques to reduce pain, improve function in the joint.
- Exercises for improving mobility, strength, and also function.
- Braces and splints for immobilization as needed.
- Post concussion therapy focusing on your symptoms and additionally presentation, which is provided by a physiotherapist trained in concussion therapy.
- Vestibular rehabilitation services provided by a physiotherapist specifically trained in vestibular rehab.
Need some help?
Your assessment session would ideally be an hour and treatment sessions would be 45 min to an hour in our clinic. Here at PhysioNow, we have many highly knowledgeable physiotherapists that can assist you with your injuries. If you think physiotherapy may help with an injury from an MVA, book with PhysioNow today for your first assessment and treatment!